Treasure Island (FL): StatPearls Publishing 2022 Jan.  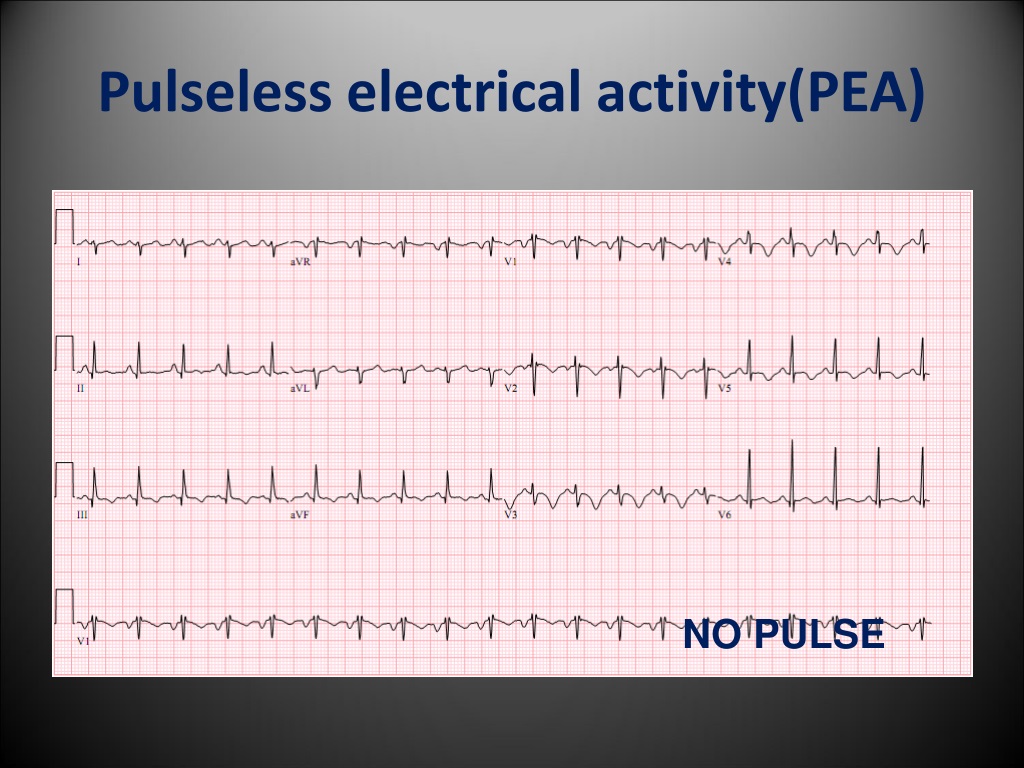 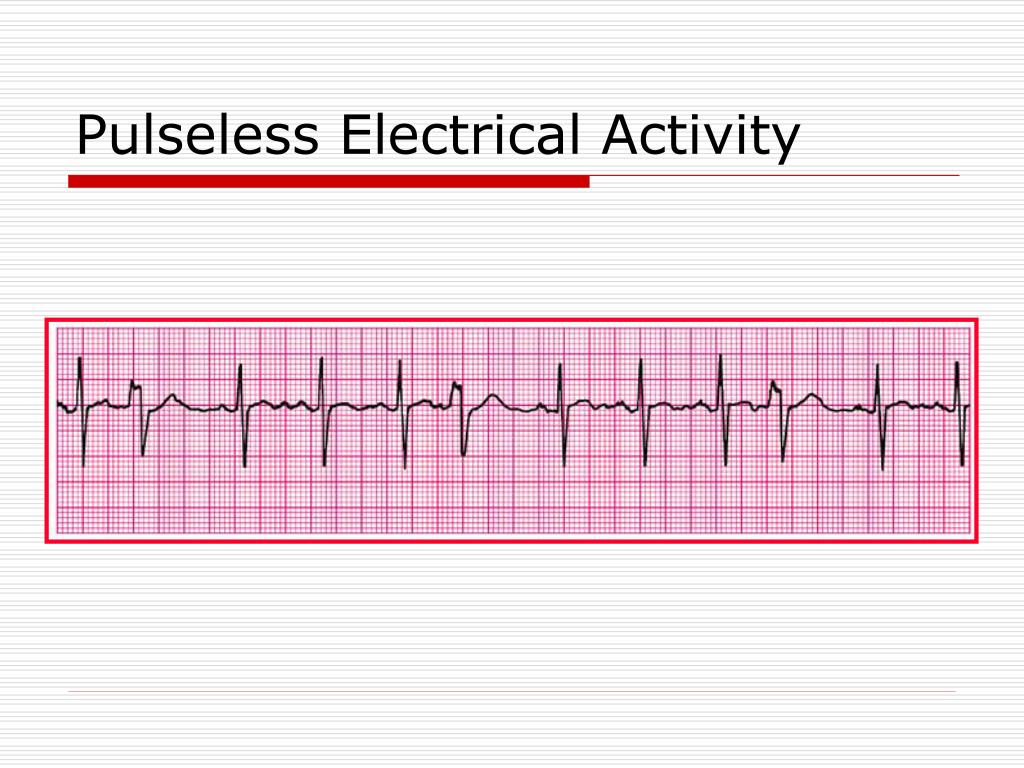
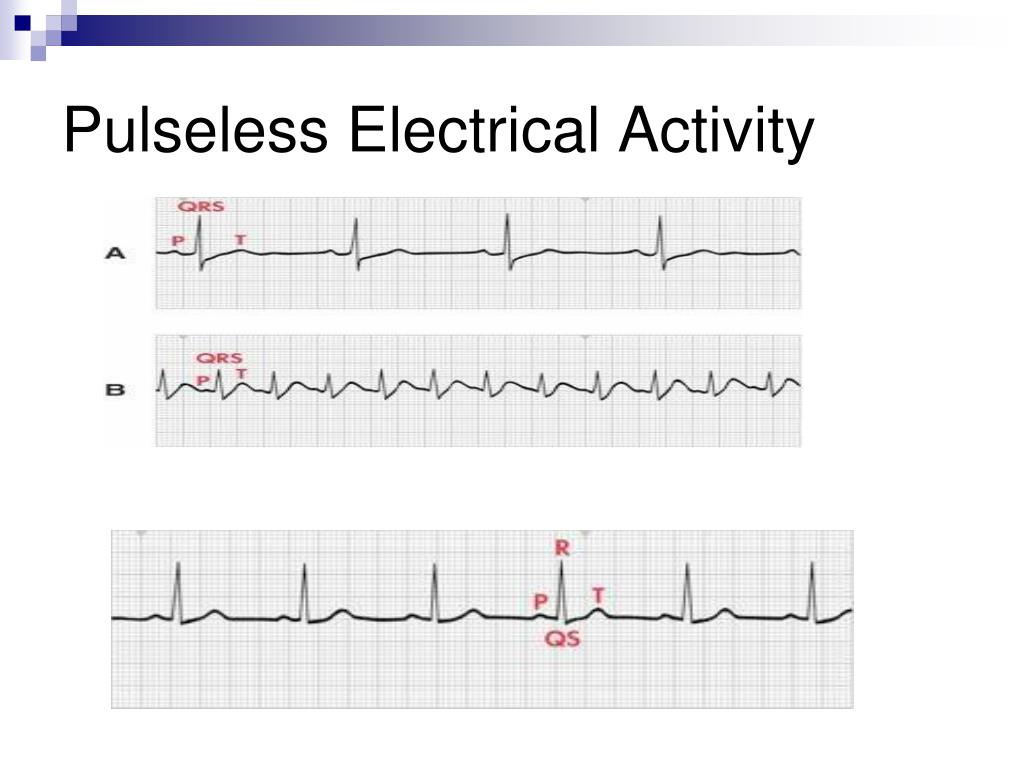
Now test your knowledge with this Pulseless Electrical Activity (PEA) Quiz.Īmerican Heart Association | Algorithms. Think of the H’s and T’s: hypovolemia, hypoxia, toxins, thrombosis and so forth. Other treatment includes supporting the airway.Īs the patient is resuscitated it’s important to think of a potential cause of the rhythm. Medications that can be administered are Epinephrine. A substantial number of PEA arrests are caused by coronary ischemia in the setting of acute coronary occlusion, but the underlying mechanism is not well understood. It’s important to note that Pulseless Electrical Activity (PEA) is a non-shockable rhythm. Pulseless electrical activity (PEA) is a common initial rhythm in cardiac arrest. When help arrives follow ACLS algorithm recommendations. tach I know PEA is when a patient has a rhythm on ECG but has no pulse. When you confirm the patient is experiencing PEA, get help by activating emergency response system (call a code blue etc.) and start CPR. How can you tell the difference on ECG between PEA & pulseless v. 4H4T, hypoxia, hypovolaemia, hypo-/hyperkalaemia, hypothermia, thromboembolism (pulmonary embolus), toxins, tension pneumothorax, tamponade (cardiac). Treatment for Pulseless Electricial Activity (PEA) Reliable causes of pulseless electrical activity (PEA) and patterns of early electrocardiogram (ECG) during resuscitation from in-hospital cardiac arrest. Hypovolemia ( shock), hypoxia, electrolyte imbalance (example high or low potassium), thrombosis, some type of trauma, cardiac disease etc. Causes of Pulseless Electrical Activity (PEA) A cardiac arrest is caused by a dangerous abnormal heart rhythm (arrhythmia), which happens when the electrical system in the heart isnt working properly. This rhythm is a great example of why you can’t always trust the ECG monitor and must check the patient for yourself. However, again when you go to check the patient, they will have NO pulse and be unresponsive. In addition, you may or may NOT see p waves and QRS complex. Our findings offer prospects for studies of the development of interventions to improve PEA survival.The organized presentation of this rhythm can vary in that you may see something on the ECG that looks like normal sinus rhythm, sinus bradycardia, sinus tachycardia etc. The implications of these findings are that PEA is a common manifestation of tissue hypoxia and metabolic substrate depletion. The process is contiuous with none of the sudden phase shifts seen in dysrhythmic events such as VF, VT or SVT. Echocardiographic images delineate the stages of pseudo-PEA with ineffective contractions, PEA, and then asystole. Introduction: Pulseless electrical activity (PEA) is an increasingly common presentation in cardiac arrest. The observation from these cases confirms that PEA is a late phase in the clinical dying process. This paper presents a small case series of individuals with brain death whose family members consented to the echocardiographic observation of the dying process after disconnection from life support. Over 30 years of studying and practicing resuscitation have allowed the authors to see a substantial rise in PEA with variable survival rates, based on the patients' illness spectrum and intensity of monitoring. Lack of clear understanding of the emergence of PEA has limited the research and development of interventions that might improve the low rates of survival typically associated with PEA. The development of monitors that can display the underlying rhythm has allowed us to differentiate between VF, asystole, and PEA. Finding individuals with no consciousness or pulse but with continued electrocardiographic (EKG) complexes obviously raises the question of how they got there. Pulseless electrical activity (PEA) is considered an enigmatic phenomenon in resuscitation research and practice. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
